What Does Acupuncture Do to the Body?
In my last post, I asked the practical question: does acupuncture work? I wrote it because a member of my family has been undergoing acupuncture, which gave the question a more personal frame. Yet once I started looking into the evidence, another question quickly took over: how acupuncture works, if it works at all. What exactly is a needle doing to the body?
Acupuncture is wrapped in ideas about qi and meridians, concepts that do not fit easily into modern biology. Yet once a needle enters living tissue, the story becomes much harder to dismiss. It can stimulate nerves, change local signaling, and send new input into the spinal cord and brain. So even if the old explanatory language does not map neatly onto anatomy, the body may still be responding in real and measurable ways.
That still does not close the case. A plausible mechanism is not the same thing as a strong treatment effect. Biology can show how something could work without telling us how much it helps in actual patients. Still, the mechanism question is worth asking, because it helps sort narrower, more credible claims from the grander ones. It also helps explain why acupuncture looks more plausible for pain and nausea than for sweeping claims about restoring whole body balance.
To understand how acupuncture works, you have to follow the signal from the needle into the nervous system itself. That means looking at sensory nerves, spinal gating, brain networks, descending pain control, and the strange fact that expectation can become part of the biology.
Two Ways of Explaining How Acupuncture Works
Two medical languages
Acupuncture comes with two very different explanatory languages. In traditional East Asian medicine, practitioners speak of qi, meridians, pattern diagnosis, and the restoration of balance across organ systems. In modern biomedicine, the terms sound very different. Researchers instead ask whether needles stimulate sensory nerves, alter spinal and brain signaling, or shift autonomic and immune activity. In this post, I am using that second approach. The goal is to examine the evidence for how acupuncture works in biological terms, while keeping the traditional framework in view as a separate medical language.
The distinction is worth making because the two systems were built for different purposes. Traditional acupuncture developed as a clinical framework for organizing symptoms and guiding treatment. Western physiology, by contrast, aims to identify measurable structures, signals, and mechanisms. So when people ask how acupuncture works, they are often moving between two maps that divide the body differently and judge claims by different standards. One map is rooted in historical medical theory. The other is rooted in anatomy, experimental physiology, and clinical evidence.
What science can say with confidence
That scientific picture of how acupuncture works comes with different levels of confidence. Some findings, such as sensory nerve activation and engagement of pain modulating systems, rest on a substantial body of work. Others still sit in the category of plausible interpretation, where the biology is suggestive but the clinical significance remains uncertain.
A narrower, testable question
For this piece, I am not trying to translate qi into nerves or meridians into blood vessels, fascia, or some newly discovered structure. That kind of one to one conversion usually creates more confusion than clarity. Instead, I am asking a narrower question: when a needle enters tissue, what detectable biological events follow? Does it activate sensory afferents? Does it trigger local chemical signals? Does it alter pain processing in the spinal cord or brain? Those are the kinds of questions that modern science can actually test.
That narrower frame leaves some questions outside the scope of a post on how acupuncture works. It does not tell us whether traditional concepts should be understood metaphorically, clinically, or philosophically. It also does not rule on the larger worldview of East Asian medicine. What it does offer is a way to evaluate specific claims with measurable evidence. If we want a scientific account of how acupuncture works, this is the place to start.
What Happens at the Needle Site
Sensory nerves are the clearest starting point
Once an acupuncture needle enters the skin, the most solid biological claim is also the simplest: it can stimulate nearby sensory nerve endings. That gives the nervous system a new stream of input to process, especially when the needle is manipulated by twisting or lifting. In other words, the needle is not inert. It acts as a controlled physical stimulus, and that makes the needle site the logical place to begin any evidence based account of how acupuncture works. Experimental reviews consistently describe activation of afferent fibers as one of the best supported parts of the mechanistic story.
Local chemistry may shift as well
Local chemistry may also change. One widely discussed example is adenosine, a signaling molecule that can dampen pain transmission under some conditions. Studies, especially in animal models, suggest that needling can raise adenosine levels near the insertion site. That finding gives acupuncture a concrete biochemical foothold, although it does not by itself tell us how much clinical benefit patients will feel. So this part of the story looks plausible and experimentally grounded, but its real world significance remains harder to pin down.
Fascia remains a more tentative idea
A third idea involves connective tissue and fascia. The hypothesis is that twisting a needle deforms local tissue and triggers mechanotransduction, setting off downstream cellular responses. This is an active area of research, and some recent work points to fibroblasts and related tissue responses as possible players. Still, this remains much less settled than simple sensory nerve activation. At this stage, fascia based explanations belong in the category of promising interpretation rather than established clinical mechanism.
So the needle site offers a believable starting point for how acupuncture works, though not a full explanation. Needling can generate real local signals, both neural and possibly chemical. What remains less certain is how strongly those local events contribute to symptom relief, and how often they do so apart from context, expectation, and the wider treatment ritual. The next question, then, is how those incoming signals are handled once they reach the spinal cord.
How Acupuncture Works in the Spinal Cord
Pain signals are filtered, not simply relayed
The spinal cord gives us the next piece of the story on how acupuncture works. Pain does not travel to the brain as a simple readout of tissue injury. Instead, the dorsal horn of the spinal cord filters incoming signals before they move upward. That is why pain researchers often describe pain as a regulated output rather than a direct measure of damage. In this framework, acupuncture becomes biologically plausible because it adds new sensory input at a key relay point where the nervous system already sorts, amplifies, and suppresses competing signals.
The pain gate still helps as a model
This is where the old idea of a “pain gate” still helps, even if the phrase can oversimplify. Low threshold input carried by larger afferent fibers can reduce the transmission of nociceptive signals carried by smaller pain fibers. The basic intuition is familiar: rub a bruised shin and it hurts less. Acupuncture may tap into a related principle, especially when needling or electrical stimulation recruits fibers that shift dorsal horn processing toward inhibition. So the spinal cord offers a concrete reason pain relief remains one of the more believable domains for acupuncture.
The evidence is strongest in controlled models
Researchers have also found more specific spinal effects, at least in animal models and especially with electroacupuncture. Studies describe reduced activity in wide dynamic range neurons, less spinal sensitization, and stronger inhibitory signaling in the dorsal horn after stimulation. Those findings do not prove that every acupuncture session in a clinic works through the same pathway. They do, however, support the larger idea that needling can alter how nociceptive information gets filtered before it reaches higher brain centers.
Even here, though, caution helps. “Spinal gating” is best treated as a useful model for how acupuncture works, not a complete explanation. Much of the cleanest mechanistic evidence comes from controlled laboratory studies, often using electroacupuncture in animals. Human pain is messier. Expectation, attention, emotion, and prior experience all feed back into the system. Still, the spinal cord gives acupuncture one of its strongest mechanistic footholds, and it helps explain why pain remains the most biologically plausible target.
How Acupuncture Works in the Brain
Pain is shaped by the brain, not just the body
Once signals leave the spinal cord, they enter a brain that does far more than register pain. The brain weighs sensation against attention, emotion, memory, and threat. That is why pain feels different when we are calm, frightened, distracted, or exhausted. Acupuncture enters that system as a sensory event, and possibly as a meaningful therapeutic event as well. So any serious account of how acupuncture works has to include brain networks involved in pain, salience, and affect.
Brain imaging offers clues, not answers
This is where brain imaging becomes interesting. fMRI and related methods often find changes in regions such as the insula, anterior cingulate cortex, prefrontal cortex, thalamus, and periaqueductal gray after acupuncture. Those areas fit what we know about pain processing and modulation. They also fit the broader idea that acupuncture can influence both sensory and emotional components of pain. Yet imaging does not tell a simple story. Many studies are small, methods vary, and the overall quality of evidence remains limited.
Context complicates the interpretation
Then comes the harder interpretive problem. A brain scan can show that something happened after needling, yet it cannot easily tell us why it happened. Was the effect driven by needle placement, tissue stimulation, expectation, therapist interaction, or the ritual of treatment itself? In practice, those factors often arrive together. That is one reason sham acupuncture can still produce measurable changes and sometimes meaningful symptom relief. The brain responds to context as well as to needles.
So the brain level story is plausible, though still incomplete. Acupuncture appears capable of engaging networks tied to pain, salience, attention, and emotion. That finding supports a real biological effect at the level of central processing. Even so, brain imaging cannot by itself settle whether specific needling carries unique power beyond expectancy and treatment context. To answer that question, we have to look more closely at the chemistry of descending pain control.
Neurochemistry and Descending Pain Control
How acupuncture works through the brain’s own pain dampening systems
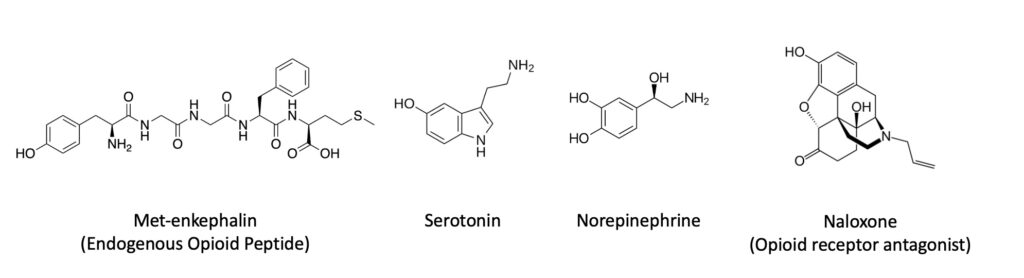
The next layer involves the brain’s own pain dampening systems. Acupuncture research has long focused on endogenous analgesia, especially opioid pathways and descending control circuits that run from the brainstem back to the spinal cord. In plain terms, the nervous system can turn pain signals down as well as send them upward. That principle is not unique to acupuncture, but it gives acupuncture a biologically credible route to pain relief. Reviews of the mechanistic literature, especially on electroacupuncture, consistently point to opioid peptides, serotonin, and norepinephrine as part of that story.
Opioids remain one of the clearest clues to how acupuncture works
The opioid piece has the longest history. Early experiments suggested that acupuncture analgesia could be reduced by naloxone, an opioid blocker, which helped make endogenous opioids a central part of the mechanistic picture. Since then, animal studies and reviews have continued to support opioid involvement, although the evidence does not imply one simple, universal pathway for every condition, protocol, or patient. The more careful conclusion is that opioid signaling appears to contribute to acupuncture analgesia in at least some settings, particularly in experimental pain models and electroacupuncture studies.
Monoamines add another layer to how acupuncture works
Monoamines add another layer. Descending serotonergic and noradrenergic pathways from the brainstem can suppress nociceptive transmission in the spinal cord, and electroacupuncture appears capable of engaging those systems as well. This helps connect the local stimulus of a needle to a broader top down modulation of pain. It also explains why electroacupuncture often shows clearer physiological signatures than very light manual needling. Electrical stimulation gives researchers tighter control over frequency and intensity, and it may recruit afferent fibers more reliably than a brief or subtle needle stimulus.
Even here, however, the evidence has limits. Much of the cleanest neurochemical work comes from animal experiments, and electroacupuncture often performs better in mechanistic studies than the gentler, more variable needling used in many clinics. So this section gives us another plausible and partly verified component of how acupuncture works, especially for pain. It does not yet give us a complete, clinic wide explanation. From there, the discussion naturally broadens to autonomic and neuroimmune pathways, where the biology becomes intriguing and the temptation to overstate it grows stronger.
Autonomic and Neuroimmune Effects
How acupuncture works beyond pain pathways
Beyond pain pathways, acupuncture may also influence stress physiology through the autonomic nervous system. That possibility has drawn a great deal of attention, because autonomic tone shapes heart rate, gut function, vascular responses, and many features of the stress response. Clinical studies often use heart rate variability as a rough window into that system. Recent meta analysis suggests modest improvement in some autonomic measures, especially SDNN, after acupuncture. At the same time, the evidence remains heterogeneous, and several key measures still show substantial uncertainty.
Autonomic circuits may be part of how acupuncture works
The broader biological idea is easy to follow. A sensory stimulus at the body surface can travel through central autonomic circuits and shift downstream output to organs and tissues. Reviews of the field describe plausible effects on sympathetic and parasympathetic balance, along with possible links to gastrointestinal and mood related symptoms. That story fits what we know about how the brain coordinates bodily state. Even so, the exact pattern depends on needle location, stimulation intensity, and disease context, which makes simple generalizations risky.
Neuroimmune pathways are more intriguing than proven
The neuroimmune story is even more intriguing. In animal work, especially with electroacupuncture, researchers have traced pathways in which somatic sensory input engages autonomic reflexes that can reduce inflammatory signaling. One influential mouse study found that low intensity stimulation at ST36 activated a vagal adrenal pathway, lowered TNF and IL 6, and improved survival in endotoxin challenged mice. That is a real mechanistic result. However, it comes from a highly controlled animal model, and it does not by itself show that routine acupuncture sessions produce comparable anti inflammatory effects in human patients.
This is where caution becomes essential. Mechanistic plausibility can tell us that a pathway exists, or that a physiological shift may occur under certain conditions. It cannot tell us, on its own, that a treatment delivers meaningful clinical benefit across a broad range of disorders. That gap is especially important in acupuncture, where immune and autonomic claims often expand much faster than the outcome evidence. So this part of the biology is worth taking seriously, while still keeping a firm distinction between what looks plausible, what has been shown experimentally, and what has actually been proven in patients.
How Acupuncture Works Through Context and Expectation
Context may be part of how acupuncture works
This leads to the uncomfortable part of the acupuncture story. The treatment context may not sit on the sidelines. It may be part of the biology. A patient lies down, focuses on bodily sensations, receives careful attention, and expects a meaningful intervention. Those conditions can change prediction, attention, anxiety, and valuation, all of which shape pain and other symptoms. In that sense, the so called placebo component is not imaginary. It reflects real psychobiological processes that alter how the brain and body respond.
Sham procedures complicate how acupuncture works in trials
That point is especially important in acupuncture because sham procedures often do more than mimic treatment. They can still involve touch, ritual, practitioner confidence, and sometimes even mild sensory stimulation. As a result, sham acupuncture can produce measurable symptom improvement, particularly in pain studies. Recent meta analyses and reviews continue to show that these context driven responses are substantial and that different sham designs can produce different sized effects. So acupuncture trials do not compare a fully active treatment to a dead control. They often compare one complex intervention with another that still does something.
Placebo is part of how acupuncture works, not a synonym for fakery
This is where the word placebo can mislead. In everyday speech, it sounds like fakery or self deception. In physiology, it points to mechanisms involving expectation, conditioning, endogenous opioids, dopamine, and shifts in brain connectivity. Those responses do not prove that specific needling is irrelevant. They do show that meaning and ritual can become biologically active parts of care. That is why the most careful question is rarely “does acupuncture beat placebo” in some absolute sense. A better question asks how much benefit comes from specific needling, how much comes from context, and whether the total effect is large enough to help patients.
Seen this way, the placebo issue becomes less embarrassing and more informative. It tells us that treatment effects can arise from multiple layers at once: sensory input, descending pain control, expectation, and the social ritual of care. Acupuncture brings those layers together unusually well, which is one reason it remains so hard to study cleanly. The challenge, then, is not to dismiss context effects as fake. It is to understand them clearly, and to decide how much of acupuncture’s clinical impact survives once those effects are taken into account.

Meridians, Anatomy, and the Problem of Translation
How acupuncture works without forcing meridians into anatomy
At this point, it becomes tempting to force a translation. If acupuncture produces measurable biological effects, then meridians must be nerves, or fascia, or blood vessels, or some hidden anatomical network. That conclusion goes too far. So far, modern research has not identified meridians as distinct anatomical structures in the way it identifies arteries, peripheral nerves, or lymphatic vessels. What it has found, more modestly, is that many acupoints lie in tissue rich regions where nerves, connective tissue planes, small vessels, and other responsive structures often converge.
Acupoints may overlap with anatomy without explaining how acupuncture works
That is a more useful way to frame the overlap. Acupoints may function as a historical coordinate system that often lands on biologically interesting terrain. In some body regions, those points line up with connective tissue planes or nerve dense areas more often than chance would predict. Still, the match is not exact or universal, and the evidence does not justify treating meridians as a simple rediscovery of modern anatomy. The scientific picture here remains suggestive rather than settled.
A respectful boundary between two ways of explaining how acupuncture works
This distinction helps keep the conversation respectful and clear. Traditional East Asian medicine developed its own clinical map of the body, one built around patterns, functions, and relationships rather than dissection based anatomy. Western science asks a different kind of question. It wants measurable structures, reproducible mechanisms, and testable causal chains. Those projects can intersect without becoming identical. When they are forced together too aggressively, both systems become harder to understand.
So the fairest conclusion is a limited one. Meridians do not need to be literal anatomical tubes or wires for acupuncture to have biological effects. At the same time, any biological account of how acupuncture works should rest on measurable mechanisms such as sensory nerve activation, local signaling, spinal modulation, and brain level processing, rather than on attempts to retrofit qi into modern physiology. That leaves room for cultural respect without lowering the standards of evidence.
How Acupuncture Works: The Bottom Line
After all of this, the most defensible biological story is also the simplest. Acupuncture appears to work as a form of structured sensory input. A needle stimulates peripheral afferents, generates local signals, and can influence spinal processing, brain networks, and descending pain control. Context then layers on top of those effects, shaping attention, expectation, and symptom appraisal. So when I ask how acupuncture works, the strongest answer points to neuromodulation, not to a hidden anatomical system waiting to be discovered.
That account also fits the broader evidence pattern. Acupuncture looks most plausible where the nervous system already plays a large role in shaping symptoms, especially pain. Nausea also remains a credible target, although the evidence is more specific than many people assume. For example, point stimulation around P6 has long shown signal in nausea and vomiting research, and a recent meta analysis in cancer care found benefit for delayed vomiting rather than acute nausea across the board. These are narrower claims than “whole body rebalancing,” but they are also more biologically and clinically grounded.
That leaves a conclusion that is less mystical and also less dismissive. Acupuncture is neither magic nor an empty ritual. It is a complex intervention that combines sensory stimulation with meaning, expectation, and care. Some parts of its mechanism are well supported. Others remain plausible but unsettled. That is why the strongest case for acupuncture stays close to conditions where modest modulation of pain or related physiology could reasonably help, while broad systemic claims still deserve a higher bar.
Your thoughts?
What do you think about the biology of acupuncture? Do you find the modern mechanistic account convincing, or do you think the evidence still leaves too many open questions? I would also be interested to hear whether you have tried acupuncture yourself, and if so, whether it seemed to help with pain, nausea, stress, or something else.
More broadly, how should we think about treatments that appear to combine specific physiological effects with powerful context effects? If a treatment changes symptoms through attention, expectation, and ritual as well as direct sensory input, does that change how you judge its value?
Share your thoughts in the comments.
Bleeding Edge Biology recommends
Websites and evidence overviews
- NCCIH: Acupuncture — Effectiveness and Safety
Start here if you want a clear, evidence based overview of acupuncture from a mainstream medical source. It gives you a grounded sense of where the evidence is strongest, where it is mixed, and what safety questions are worth keeping in mind. - NCCIH: Traditional Chinese Medicine — What You Need To Know
This is useful if you want a broader look at the larger system that acupuncture comes from. It helps place acupuncture in the context of traditional Chinese medicine without asking you to accept its claims uncritically. - Cochrane: Acupuncture for Chronic Non-Specific Low Back Pain
Read this if you want to see how cautious evidence reviewers handle acupuncture. It is especially useful because it shows how a treatment can look somewhat helpful while still raising questions about clinical significance and study design.
Review articles and key papers
- Fan et al., “Effects and mechanisms of acupuncture analgesia mediated by afferent nerves in acupoint microenvironments”
If you want to understand the local biology, this is a strong place to begin. It walks you through what may happen at the needle site, including nerve activation and the tissue level events that could help shape pain signaling. - Wang et al., “Neural circuit mechanisms of acupuncture effect: where are we now?”
This review is useful if you want the modern neuroscience version of the story. It looks at acupuncture through brain and nerve circuits rather than through meridians, which makes it a good companion to the argument in this post. - Goldman et al., “Adenosine A1 receptors mediate local anti-nociceptive effects of acupuncture”
This is one of the landmark mechanistic papers. Read it if you want a concrete example of how a needle could trigger a measurable biochemical effect in local tissue rather than just a vague claim about “energy.” - Kim et al., “Effectiveness and Safety of Acupuncture for Nausea and Vomiting in Cancer Patients”
This one is helpful because it focuses on a narrower and more plausible clinical use of acupuncture. If you want to see how the evidence looks when the claims are more specific, this is a good example.
Books
- Ted J. Kaptchuk, The Web That Has No Weaver: Understanding Chinese Medicine
Pick this up if you want to understand Chinese medicine in its own terms rather than through a forced Western translation. It gives you a much better feel for how practitioners think about qi, patterns, and diagnosis. - Simon Singh and Edzard Ernst, Trick or Treatment? The Undeniable Facts about Alternative Medicine
Read this if you want the skeptical counterweight. It is especially useful for keeping separate two questions that often get blurred together: whether a mechanism sounds plausible and whether a treatment actually helps patients in rigorous trials.
Talks and videos
- Ted Kaptchuk, “Placebo Effects Make Good Medicine Better” (TEDMED)
Watch this if you want a smarter way to think about placebo effects. It will help you see why ritual, expectation, and the clinical encounter can produce real physiological changes without reducing the whole treatment to fakery. - Emma Bryce, “The Power of the Placebo Effect” (TED-Ed)
This is a quick and accessible introduction to placebo biology. It is a good choice if you want the basic idea in plain language before digging into sham acupuncture trials. - The Science of Acupuncture — BBC Documentary
Watch this if you want a longer, more visual introduction to the acupuncture debate. It follows physicist Kathy Sykes as she looks at acupuncture in both clinical and cultural contexts, including its use in China and the effort to test it scientifically.